Self-funding you company’s healthcare plan has a lot of upsides, including more flexibility, happier, healthier employees, and big potential savings. But one thing that can give businesses pause when they consider making the switch is the underlying financial risk. By taking on the responsibility to fund your employees’ healthcare, you’re ultimately putting yourself on the hook for all the claims that arise when your employees use their healthcare benefits. And as everyone knows, health and healthcare can be very unpredictable—just one member getting diagnosed with a chronic disease, for example, could mean expensive ongoing treatment that increases care claims significantly.
If your company’s plan is self-funding, those kinds of unexpected, unpredictable, claims could be a real financial risk, adding an element of uncertainty to your finances that you’d rather avoid. Fortunately, there’s a powerful tool you can use to limit your exposure to unexpected healthcare costs; medical stop-loss insurance.
So what is medical stop-loss insurance? At its most simple, medical stop-loss is a kind of insurance against catastrophically high medical claims, limiting the amount a self-funded health plan must pay when claims exceed a certain amount.
Of course, like any insurance product, the details get more complicated the more you dig in, and there’s plenty of jargon to understand before you can call yourself an expert! Below, we’ll walk through the basics, explore the key terms you need to know and show you how stop-loss medical insurance can help your business control the potential risks of self-funding.
“medical stop-loss is a kind of insurance against catastrophically high medical claims, limiting the amount a self-funded health plan must pay when claims exceed a certain amount.”
Medical Stop-Loss Basics
Imagine that you’re in charge of building a self-funded healthcare program at a medium-sized company. Assuming everyone stays health year over year, you’d probably have a pretty good idea of how much care will cost moving forward, and you can make arrangements to have that money in place when it’s needed. Now imagine one of your plan members gets a cancer diagnosis, requiring hundreds of thousands of dollars’ worth of medicine and care. If you’re self-funding without any kind of medical stop-loss insurance on your spending, payment of those high-cost claims will fall solely on your business, potentially leading to a serious cash crunch.
Medical stop-loss insurance protects against this by setting a limit to how much your company will have to spend on claim costs in a given plan year, much like how deductibles and spending limits work in individual healthcare plans. You make a contract with an insurance company, agreeing to pay regular premiums in exchange for them taking on the risk of paying any claims over the limit you agree to.
For example, let’s say your stop-loss deductible is set at $100,000. This means your company is responsible for paying the first $100,000 of an individual employee’s healthcare claims in a given year. If that individual employee’s medical claims reach $150,000, your specific stop-loss insurance would reimburse you for the $50,000 above your deductible.
With specific stop-loss coverage, your financial exposure for any one individual is limited to the deductible amount plus the cost of your stop-loss premiums, both of which may change from year to year. While you’ll still need to budget for claims up to the deductible and for your insurance premiums, stop-loss insurance protects your company from the financial impact of unusually large claims.
This makes financial planning more predictable and shields your business from catastrophic healthcare claims, allowing you to focus on providing quality care for you employees rather than worrying about unexpected expenses.
Key Stop-Loss Terms
Now that we’ve walked through the basics, it’s time to dive into the complexity. Here are the key terms and concepts you need to know to get the full picture of how stop-loss works.
Specific coverage vs. aggregate coverage
These terns refer to how deductibles and spending limits are set in your stop-loss contract. Contracts can include one or both kinds of coverage, depending on he company’s needs.

Specific coverage protects your business against the risk of particular claims being too high, setting a spending level for each individual or family on the plan, and reimbursing you if claims rise above that. So, with a contract providing specific coverage of $100,000, you’ll be reimbursed the difference any time an individual member’s claims—including covered family claims—rise above $100,000, just like our earlier example. Specific coverage generally only applies to medical and pharmacy claims.
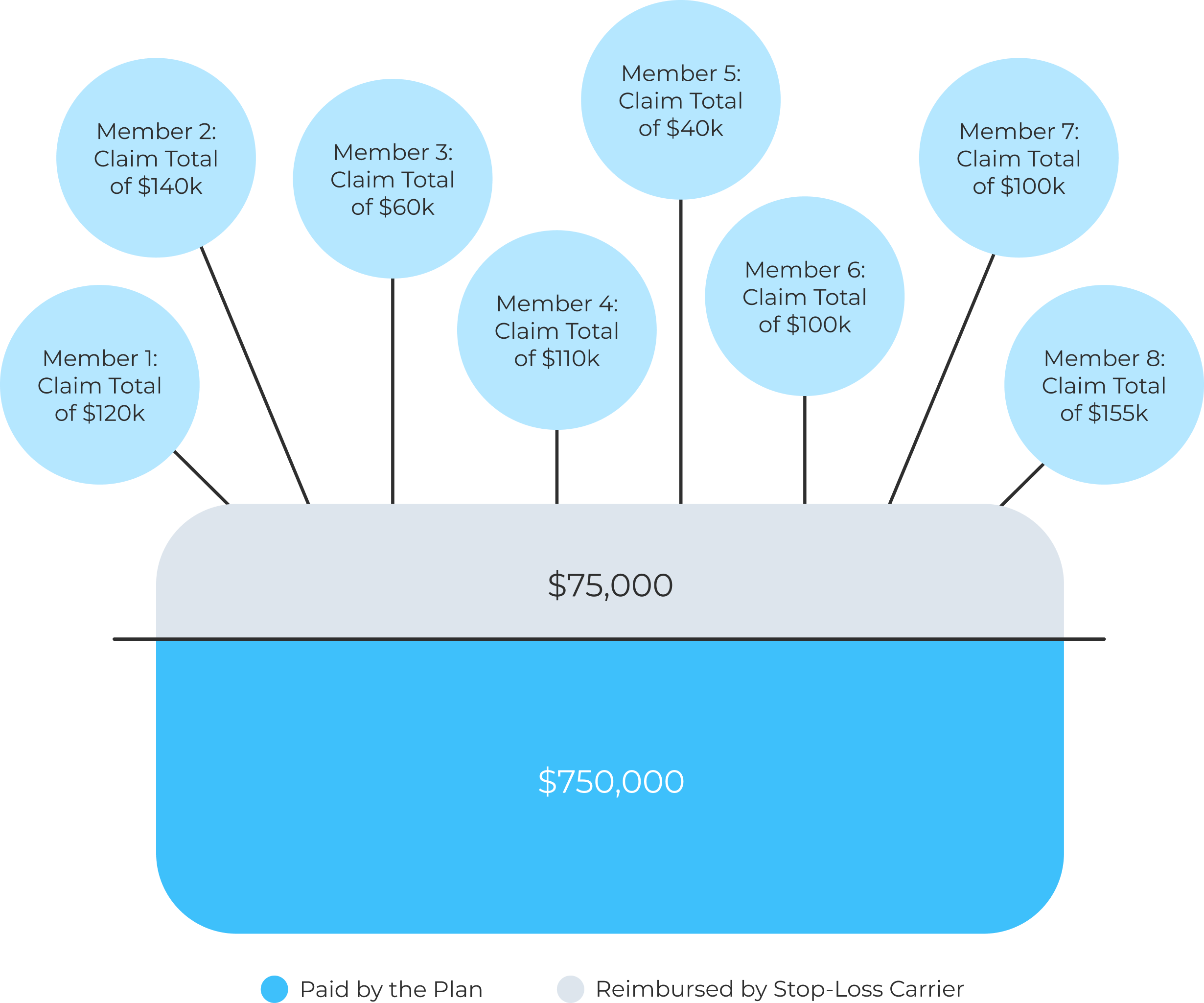
Aggregate coverage, on the other hand, is a spending limit for your entire healthcare plan. It combines all claim cost from all members into one big bucket and reimburses you if spending goes over a limit called the aggregate attachment point. This point is calculated based on projected claim costs, plus a risk corridor to account for unexpected claims. Aggregate coverage typically applies to a broader range of claims—including medical, dental, vision, pharmacy, and short-term disability.
These two types of stop-loss coverage can work together to limit financial risk, but they reimburse different types of claims and never overlap. With specific coverage, you pay claims up to the individual deductible, and then the stop-loss insurer reimburses any excess. With aggregate coverage you pay all claims up to each individual’s deductible across the plan year. If total claims (excluding any amounts already reimbursed under specific coverage) go over the aggregate attachment point, the insurer reimburses the excess. You’re never reimbursed twice for the same dollar of claims. Specific and aggregate coverages complement each other—but always stay in their lanes.

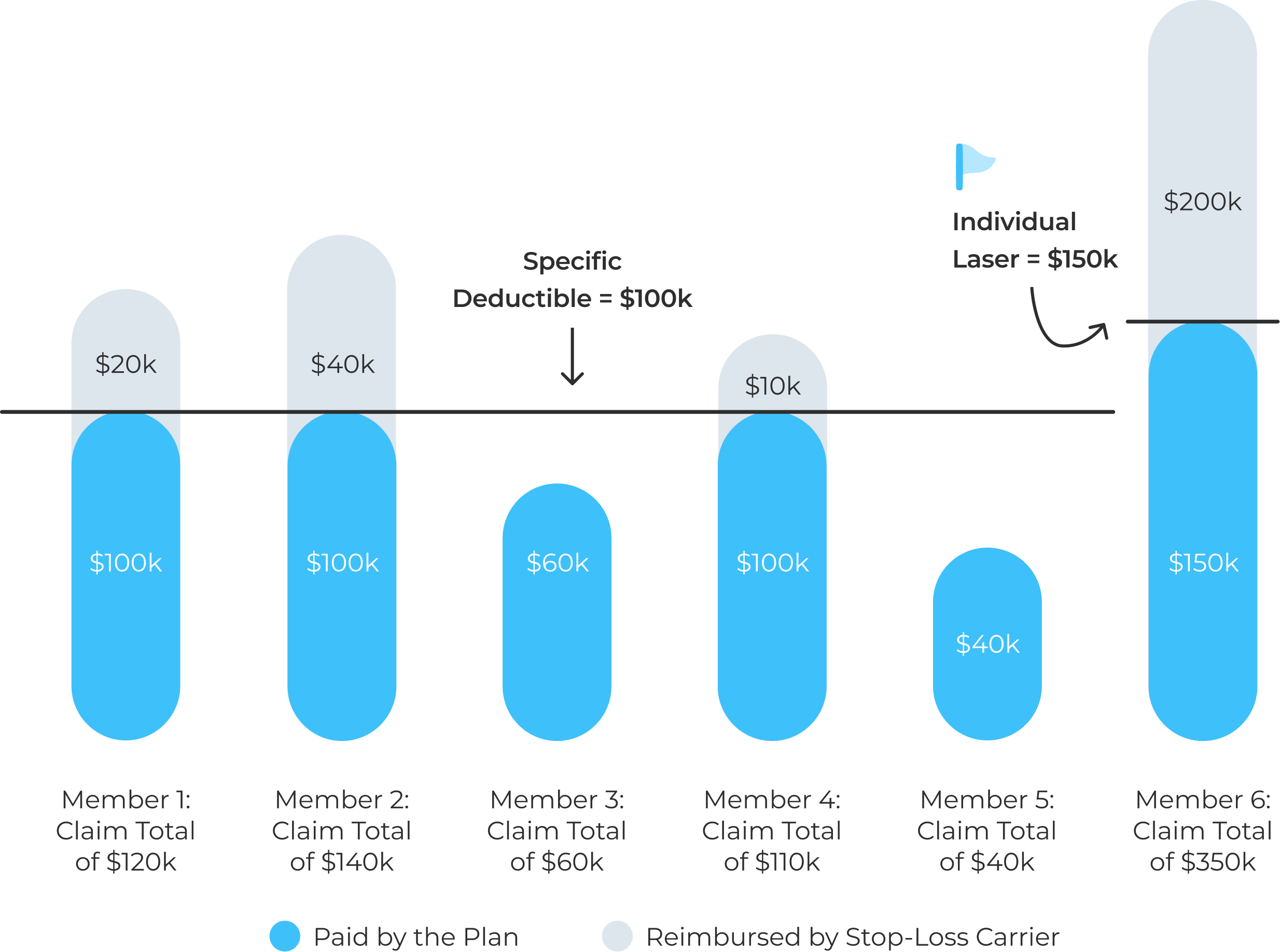
Lasers
Formally known as “individual specific deductibles”, lasers are provisions added to stop-loss contracts to control the risk taken on by the stop-loss insurer. Essentially, a laser sets a higher deductible on an individual with higher expected claims—someones requiring major surgery or dealing with a chronic illness, for example. Returning to our earlier example with specific stop-loss coverage of $100,000, an employee needing regular kidney dialysis might be subject to a laser, bumping their individual specific deductible up to $150,000. That would mean your company needs to pay the additional $50,000 before a reimbursement claim could be filed for the individual. This additional amount is not applied to the aggregate.
Margin
Margin (also called “corridor”) is the difference between expected paid claims and the attachment point, and it represents the financial risk the self-funding company is taking on with their policy. The larger the margin, the more cost the company might have to pay themselves if spending is higher than expected. That means less risk for the stop-loss provider and lower premiums for the self-funding company. Generally, stop-loss providers use a margin of around 25% of expected billings, meaning a company would have to pay 25% more than their expected claims before they hit their aggregate attachment point and their stop-loss coverage kicked in.
To see how that works with real numbers, imagine a plan with $1M in expected billings. A standard 25% corridor would mean a margin of $250,000. Taken together, that would mean an aggregate attachment point of $1.25M, so the business would have top spend that amount before their aggregate stop-loss coverage started to pay.
Contract Basis
Contract basis describes the way you and your insurer determine which claims are covered by the stop-loss insurance. Contract basis is usually expressed as two numbers representing the date a covered care event can be incurred and when it needs to be paid.
Date incurred indicates when a medical care event actually takes place—the date when a member gets surgery or fills a prescription, for example. Date paid, on the other hand, represents when the insurance policy actually cuts the check to pay for the care that has taken place.
So, for example, a 12/12 contract basis means every claim that is both incurred and paid for over the 12-month period of the contract is covered. However, imagine one of your members had surgery a month before the contract came into effect—in that case, the claim won’t be covered and you won’t be reimbursed, even if you pay for the procedure during the life of the contract.
To avoid problems like these, a variety of different contract bases are available, like 15/12: This would also cover claims incurred in the three-months before the contract, so long as they were paid during the contract’s 12-month period. Another common example is 12/15, covering any claims incurred over 12 months, so long as they are paid within three months of the end of the contract.
At the end of the day, you just want to be sure that your claims will be covered, so it’s important to negotiate contract basis that doesn’t leave you exposed to uninsured periods—remember, that you have the final responsibility to pay members care costs, and without stop-loss, those costs can be arbitrarily high.
Medical Trend
Put simply, medical trend is the estimate of how much healthcare costs are expected to rise over the next policy year due to factors like inflation, new treatments, etc. Stop-loss insurers look at trends every year to forecast how much costs will rise, raising their own premiums to offset the difference.
One very important thing to keep in mind is that premium increases will almost always be higher than medical trend taken by itself. That’s because of a dynamic called “levered trend”, which causes cost increases to fall disproportionately on the stop-loss insurer. To understand why that is, imagine a stop-loss policy with specific coverage of $100,000 and a member who had $110,000 in medical expenses last year. Now imagine medical trend is determined to be 10%—that means that member’s expenses can be projected to be 10% higher, too, coming out to $121,000. But if the specific coverage level doesn’t change, the stop-loss insurer would have to pay $21,000 instead of $10,000, an increase of 110%.
So, holding everything else equal, medical trend is amplified when it comes to stop-loss insurers’ risk, and they tend to offset that risk by raising premiums above what medical trend itself would indicate. That means that keeping you coverage levels constant will keep premiums manageable, companies can negotiate a higher deductible with their stop-loss provider, taking some of the financial risk back and lowering their premiums in return.
Underwriting Medical Stop-Loss Insurance
So, how do stop-loss insurers actually assess your healthcare plan’s risk and set premiums? Like all underwriting, it’s a complicated process, but there are a number of common factors they’ll almost always consider:
Industry
If your industry has higher than average health risks—because it involves physical labor, for instance—your expected claims will likely be higher, meaning higher premiums too.
Demographics
The age, gender and location of your plan members help underwriters predict healthcare usage and costs.
Benefit Design
Giving your plan members more benefits or lowering their deductibles increases the plan’s financial risk, which will be reflected in your premiums.
PPO Network
Depending on the care quality and discounts offered by your provider network, underwriters might expect your claims costs to be higher or lower than average.
Monthly Claims Experience
Recent claims data helps underwriters gauge your ongoing and future risk.
Specific Level
The specific deductible you choose for individual or family coverage directly affects premiums, with lower deductibles leading to higher premiums.
Pre-Certifications and Large Case Management Reports
Evidence of strong cost containment and care management can improve underwriting outcomes and lower premium costs.
Large Claims Reports and Loss Ratio
Your history of high-cost claims and your overall loss ratio indicate the likelihood of future large claims.
Ongoing Claims
Active high-cost or chronic claims increase risk and may affect rates and coverage terms or lead to lasering.
Factors like these are combined using proprietary actuarial models to determine the underlying risk of a plan. From there, underwriters are able to set premiums and decide on appropriate coverage terms for your plan’s stop-loss insurance.
How Your TPA Can Help
As we’ve seen, stop-loss can be a complicated topic, and there are lots of wrinkles to wrap your head around. Fortunately, self-funding companies don’t have to figure out stop-loss on their own—third-party administrators (or TPAs) can help you navigate the stop-loss journey from start to finish, steering you towards the right insurance partners, helping you negotiate contracts, and working with you and the stop-loss insurer to keep things running smoothly year to year.
.png)
